Incontinence is one of those topics many people find difficult to talk about. Yet it affects over 3 million adults across Britain, becoming more common as we age or face certain health conditions. If you or someone you care for is dealing with bladder or bowel control issues, you might be wondering what help is available. The good news is that the NHS does provide free incontinence pads and products for those who qualify, and there are many ways to manage the condition whilst maintaining comfort and dignity.

This guide explains everything you need to know about accessing NHS-funded incontinence pads, understanding the eligibility criteria, and finding practical strategies for day-to-day living.

How to Get Free Incontinence Pads on the NHS
Eligibility criteria
The NHS does provide free incontinence products, but eligibility varies depending on where you live. Each local Integrated Care Board (ICB) sets its own criteria, creating what many call a “postcode lottery” in provision.
Generally, you will need to demonstrate moderate to heavy incontinence to qualify. The NHS typically does not provide products for light incontinence, expecting people to purchase these themselves from supermarkets or pharmacies. You will also need to have a new or long-term condition causing the incontinence, and your self-care abilities will be assessed.
The assessment process
The first step is contacting your GP or local continence service. In some areas, you can refer yourself directly without going through your doctor.
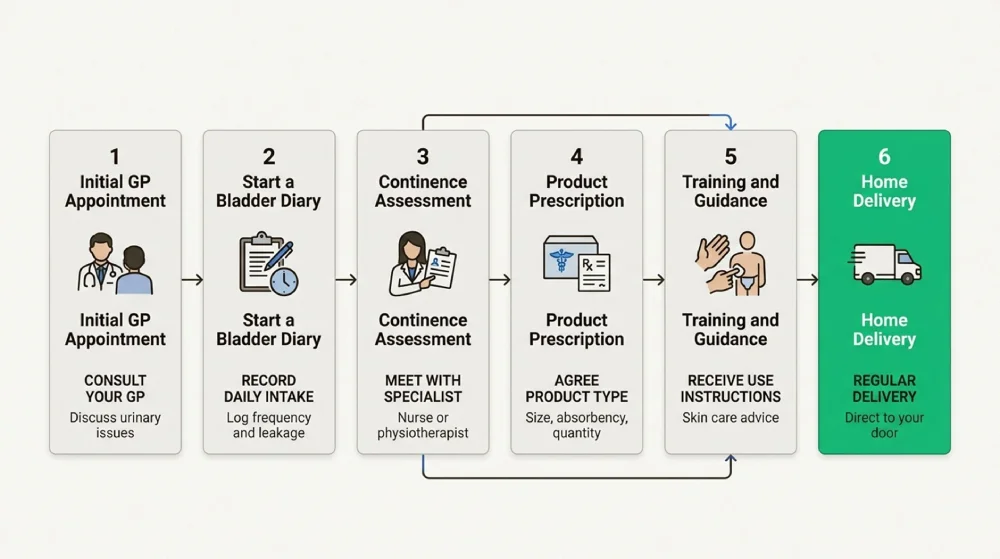
Here’s how the process usually works:
- Initial contact: Phone your GP surgery or local continence clinic to request an assessment
- Bladder or bowel diary: You’ll be asked to keep a diary for about 2 days, recording when you go to the toilet, any leaks, and what you drink
- Clinical assessment: A continence specialist nurse will review your symptoms, medical history, and current fluid intake
- Possible tests: You might need a urine test to check for infection, a bladder scan, or a physical examination
- Treatment discussion: The nurse will explore treatment options before considering pad provision
- Product delivery: If eligible, pads will be delivered directly to your home, usually on a regular schedule
What to expect at your appointment
The continence nurse will ask detailed questions about your symptoms: what type of incontinence you experience, how often leaks occur, how much urine you lose, and what products you currently use. They’ll review your medical history and medications, as some drugs can affect bladder function.
You will likely receive advice on pelvic floor exercises or bladder training techniques. The nurse will also assess your home environment and mobility to ensure any products provided will be suitable and safe for you to use.
How many pads will you receive?
Most people receive between 3 and 4 pads per day, based on their assessed clinical need. The exact number depends on the severity of your incontinence and your individual circumstances. Your allocation will be reviewed annually as a minimum, or sooner if your needs change significantly.
What NHS Incontinence Pads Are Like (and Their Limitations)
Types of products available
NHS-provided pads are typically high-absorbency disposable products designed for moderate to heavy incontinence. The total absorbency can range from 800ml to 2500ml, though you’ll usually change the pad when it reaches about 40% capacity (the “working absorbency” of 400-950ml).
For men, the NHS can also provide sheaths (condom-style devices that collect urine into a bag) and handheld urinals. Some areas offer washable reusable products, though this varies by region. Bed and chair protectors may also be available.
NHS pad limitations
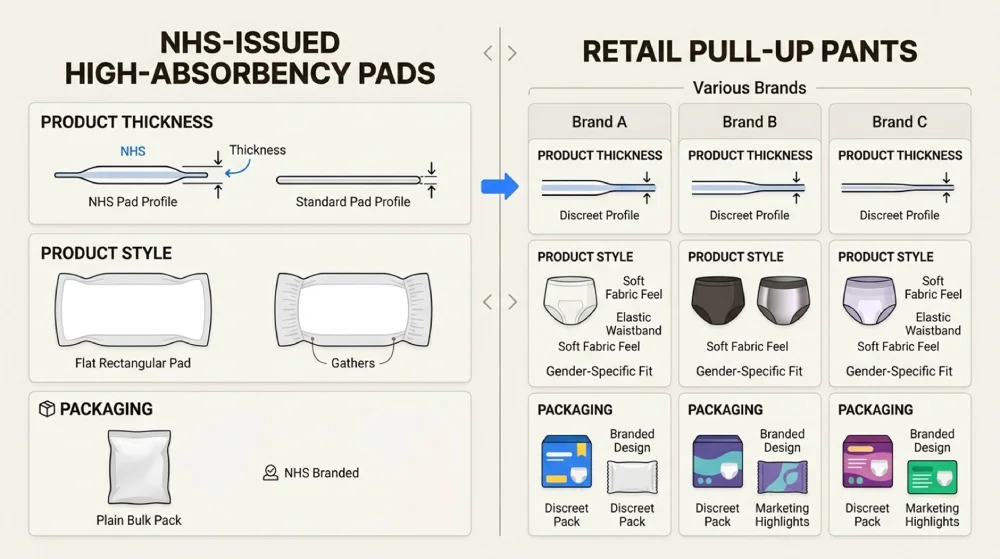
It’s important to have realistic expectations about NHS provision. The products available are limited to whatever your local NHS has contracted to supply you cannot choose from the full range available in shops. These pads tend to be bulkier than premium retail alternatives because they’re primarily designed for moderate to heavy incontinence.
Quantity restrictions apply, with most areas capping provision at 4 pads per day. Assessment waiting times can stretch to several weeks in some regions. The products may not be as discreet or comfortable as those you can buy yourself, and styles are limited compared to retail options.
What the NHS won’t provide
The NHS does not supply small pads for light incontinence, sanitary towels (which are designed differently and won’t work effectively for urine), or products for bodily fluids other than urine and faeces. Premium branded retail products are also not available through NHS provision.
Treatment Options to Reduce or Eliminate Incontinence
Conservative treatments (first-line)
Before or alongside pad provision, the NHS will usually recommend trying treatments that address the underlying cause of incontinence.
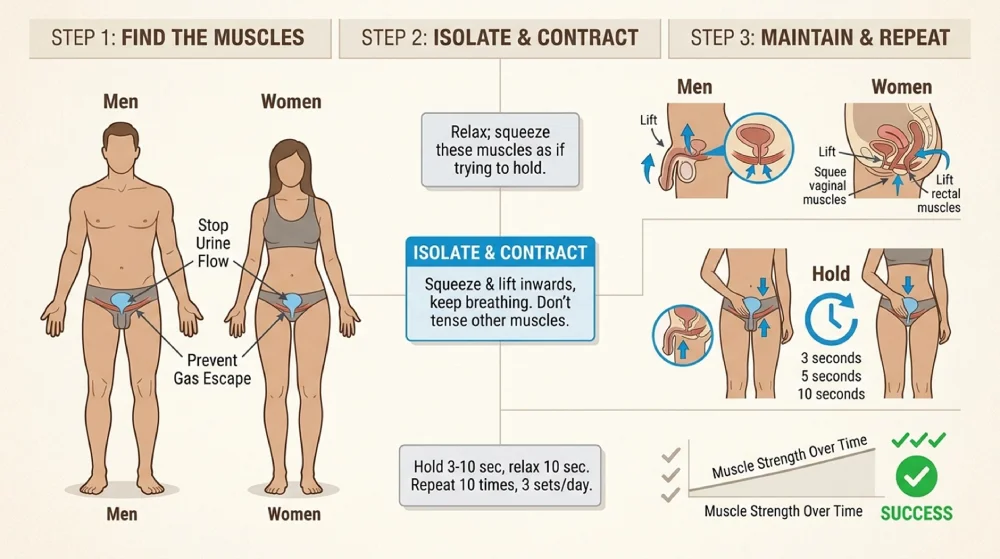
Pelvic floor exercises strengthen the muscles that control urination. A typical programme involves 8 muscle contractions, performed 3 times daily, for at least 3 months. NHS guidance confirms these exercises can benefit everyone with urinary incontinence, regardless of the cause.
Bladder training helps with urge incontinence by gradually increasing the time between feeling the need to urinate and actually going. This structured programme usually lasts at least 6 weeks.
Lifestyle changes can make a significant difference. Reducing caffeine (found in tea, coffee, and cola) helps because caffeine increases urine production. Managing fluid intake, losing weight if you’re overweight, and treating constipation all support better bladder and bowel control.
Medical treatments
If conservative treatments aren’t sufficient, several medications can help. For urge incontinence, antimuscarinics (also called anticholinergics) such as oxybutynin or tolterodine relax the bladder muscle. Mirabegron offers an alternative for those who can’t take antimuscarinics.
For stress incontinence, duloxetine can increase muscle tone around the urethra. Surgery may be recommended if other treatments haven’t worked.
When pads are appropriate
Pads serve an important role whilst you’re waiting for diagnosis, during treatment, or for long-term management when treatments haven’t fully resolved symptoms. They’re also essential for end-of-life care and temporary support during recovery from illness or surgery.
Practical Tips for Living Well with Incontinence
Pad usage best practices
Using pads correctly helps prevent leaks and protects your skin. Change your pad when the wetness indicators show it has reached about two-thirds capacity most pads have lines that change colour when wet. Never wear two pads at once; this doesn’t increase absorbency and can cause skin damage from the hard edges.
Pads can be worn overnight if the absorbency is adequate and there’s no faecal soiling. However, change immediately after any bowel movement. Most people find they need 3 to 5 pad changes per day.
Skin care and hygiene
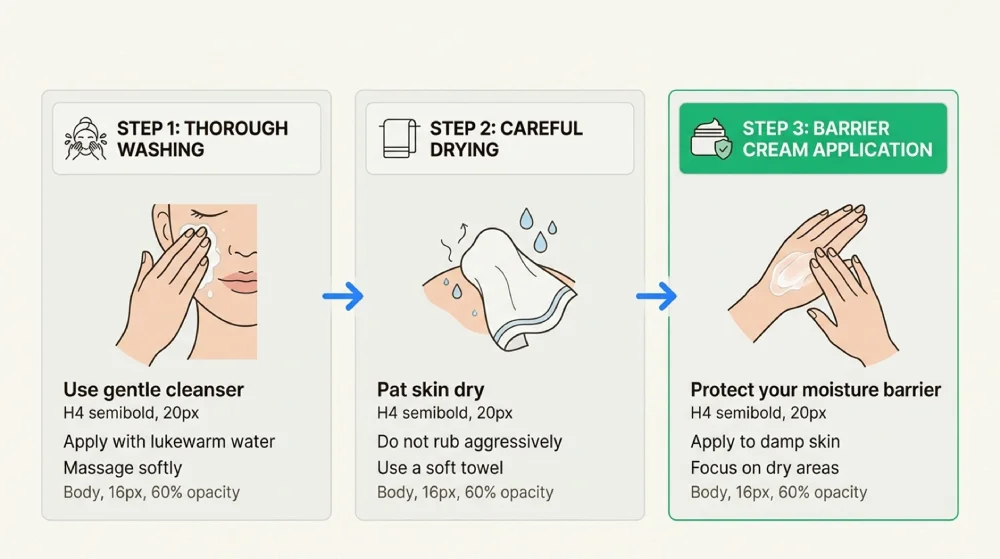
Good skin care prevents soreness and infection. Wash and dry the skin thoroughly at each pad change. Avoid talcum powder, which can inhibit the pad’s performance and create a paste when mixed with moisture. Use barrier creams only as advised by healthcare professionals.
Watch for signs of skin breakdown: redness, soreness, or raw areas. Seek medical advice promptly if skin becomes damaged, as this can lead to infection.
Staying hydrated is crucial despite fears about leakage. Aim for 1.5 to 2 litres of fluid daily (6 to 8 cups). Concentrated urine actually irritates the bladder more and can worsen incontinence.
Daily living strategies
Simple adjustments to clothing and routine can make a significant difference. Choose trousers and skirts with elasticated waists or Velcro fastenings rather than zips and buttons. When planning outings, identify toilet locations in advance and carry spare pads and a plastic bag for disposal.
The Bladder & Bowel UK charity offers a “Just Can’t Wait” card that you can show when you need urgent access to a toilet. This discreet card explains that you have a medical condition and can help you avoid queues.
For bed protection, consider waterproof mattress covers and washable bed pads. These protect your mattress and can be more comfortable than plastic sheeting.
Dietary and lifestyle advice
Maintaining adequate fluid intake is essential don’t restrict fluids to try to reduce leakage. Reduce caffeine and alcohol, which irritate the bladder. Eat plenty of fibre-rich foods (aim for 30g daily) to prevent constipation, and stay active as regular movement supports healthy bowel function.
NHS Provision in Care Homes and Supplementing Your Supplies
Rights for care home residents
If you live in a nursing home, continence products should be provided as part of your nursing care without separate charges, according to guidance from the Bladder & Bowel Community (though the overall fee may reflect your care needs). Residential home residents are entitled to NHS district nursing service provision, including continence assessments and products.
The same assessment process applies, and you have the right to request this if it isn’t offered. Family members can advocate for proper continence care by speaking with care home management or contacting the local continence service or PALS (Patient Advice and Liaison Service) if concerns arise.

When you might need additional products
Many people find that NHS provision, whilst helpful, doesn’t meet all their needs. You might want more pads than the NHS allocation allows, or prefer more discreet and comfortable options for social occasions. Light incontinence that doesn’t qualify for NHS support still requires management, and you might need products whilst waiting for your NHS assessment.
Purchasing options
Supermarkets and pharmacies stock basic incontinence products with the advantage of immediate availability. Online suppliers typically offer a wider choice, better value, and discreet home delivery.
The Continence Product Advisor website, recommended by the NHS, provides independent, evidence-based guidance on choosing products. Many suppliers offer free samples, allowing you to try different options before committing to a purchase.
When selecting products, consider your absorbency needs, comfort, discretion, and ease of use. Trial different styles pads, pull-up pants, and all-in-one slips suit different lifestyles and levels of mobility. Balance cost against quality and effectiveness, and don’t hesitate to seek advice from continence nurses even for self-funded products.
Getting Support and Further Information
NHS services
Your GP can refer you to local continence clinics, or you might be able to self-refer depending on your area. District nursing services and specialist bladder and bowel services provide expert assessment and ongoing support.
Charities and support organisations
Bladder & Bowel UK offers independent product advice and support. Call their helpline on 0161 214 4591.
Age UK provides advice for older people and carers. Their helpline is 0800 055 6112.
The Bladder & Bowel Community offers information sheets and a support network. Contact them on 01926 357220.
Continence Product Advisor provides evidence-based, independent guidance on choosing and using products.
How Serene Care Group can help
At Serene Care Group, we understand that incontinence care is about far more than just providing products. Our care homes deliver dignified, personalised continence support that respects each resident’s preferences and maintains their quality of life.
We work closely with NHS continence services to ensure our residents receive appropriate assessments and products, whilst supplementing with additional supplies when needed to ensure comfort and dignity. Our person-centred approach means we take the time to understand each individual’s needs and routines.
If you’re considering residential care for yourself or a loved one, or if you’re navigating the care system and need guidance, we’re here to help. Contact us or call 0203 758 7308 to learn more about our approach to continence care and how we support our residents to live with comfort and dignity.
Frequently Asked Questions
How long does the NHS incontinence pad assessment take?
The assessment itself usually takes 30-60 minutes. However, waiting times for appointments vary by area and can range from a few weeks to several months. Keeping a bladder diary before your appointment (typically for 2 days) helps speed up the process.
Can I choose which NHS incontinence pads I receive?
Generally, no. The NHS provides products from a local formulary a limited list of contracted suppliers. The specific products available depend on which company holds the contract in your area. If you find the supplied pads unsuitable, discuss this with your continence nurse who may be able to adjust the type within the available range.
Are NHS incontinence pads free for everyone over 65?
No, age alone doesn’t qualify you for free pads. Eligibility depends on the severity of your incontinence and local criteria. Light incontinence, which is common with ageing, typically doesn’t qualify for NHS provision regardless of age.
What should I do if NHS incontinence pads leak at night?
Contact your continence nurse for a reassessment. You may need a higher absorbency product, or there might be a fitting issue. Using a waterproof mattress protector and considering a bed pad can provide additional security whilst you sort out the underlying issue.
Can care homes charge extra for NHS incontinence pads?
Nursing homes should not charge separately for continence products as these should be included in nursing care. However, the overall fee may be higher for residents requiring this level of care. Residential home residents are entitled to NHS district nursing services including continence products. If you’re being charged separately, contact your local PALS service for advice.
How do I reorder NHS incontinence pads once approved?
Once approved, pads are usually delivered automatically on a set schedule (often monthly). If you need to reorder or change your delivery, contact the supplier directly using the details provided when you were first approved, or speak to your continence nurse.

